When the clinician has diagnosed BPPV, the clinician has likely ruled out more dangerous etiologies of dizziness it is crucial to communicate with the patient to assuage their fears because many patients present concerned about the more dire causes of dizziness, such as an intracranial mass or a stroke. However, patients have described them as lasting much longer due to associated nausea and disequilibrium. These attacks can last for under one minute. The classic symptoms of BPPV often include sudden onset vertigo, worsened by head movements. History and physical exams are pertinent in diagnosing BPPV correctly. Other common causes include head trauma and inner ear surgeries, which can often dislodge otoliths into the semicircular canals. However, other inner ear pathologies such as Meniere disease and even migraines have links to BPPV. The most common cause of BPPV is primary or ”idiopathic” as BPPV itself is often found in isolation. The classic symptoms of BPPV often involve brief episodes of rotational vertigo that are reproducible. When the vestibular apparatus, semicircular canals, and visual system are in disequilibrium, it elicits the sensation of dizziness. These otoliths move due to gravity as the head is turning and cause inappropriate signaling that the head is moving when, in reality, it is not. The majority of these otoliths can be found in the posterior semicircular canal, followed by horizontal (lateral). The disease process appears to be caused by otoliths that become displaced in the semicircular canal. Below are several definitions from the Committee for Classification of Vestibular Disorders to clarify these symptoms:īPPV is among the most common inner ear disorders that cause dizziness or vertigo. Therefore, a committee was formed to promote the classification of vestibular disorders. The language utilized to describe terms such as ”dizziness” or ”vertigo” can often mean many different things based on one’s interpretations. Symptoms and disease definitions are essential for professional communication between providers, whether they treat patients in the clinic, emergency department, or inpatient setting. Therefore, it is important to perform a thorough history, and physical exam as the ultimate diagnosis can be benign or life-threatening. Some studies have shown up to 15% of cases of dizziness in the emergency department are life-threatening. The differential diagnosis for dizziness encompasses numerous body systems, such as neurological, cardiovascular, or hematologic. peripheral.” Dizziness can account for approximately 5% of walk-in clinics and roughly 4% of emergency department visits. One critical step for providers is to characterize dizziness as “central vs. This difficulty in communication can result in frustration for both the patient and the provider however, differentiating these symptoms is critical for the provider to treat the patient effectively. When a patient complains of “dizziness,” they could be describing vertigo, pre-syncope, balance issues, or giddiness. Additionally, dizziness can be difficult for patients to describe, as it can mean different things to different people. It affects people of all age ranges with varying degrees of symptoms and severity.

The proposed new manoeuvre is simple, effective and safe for treating patients with benign paroxysmal positional vertigo and cervical spine problems.Whether one is a seasoned clinician or a medical student, dizziness can be difficult to diagnose and treat. All seven were relieved of their symptoms after undergoing the new particle repositioning manoeuvre again.
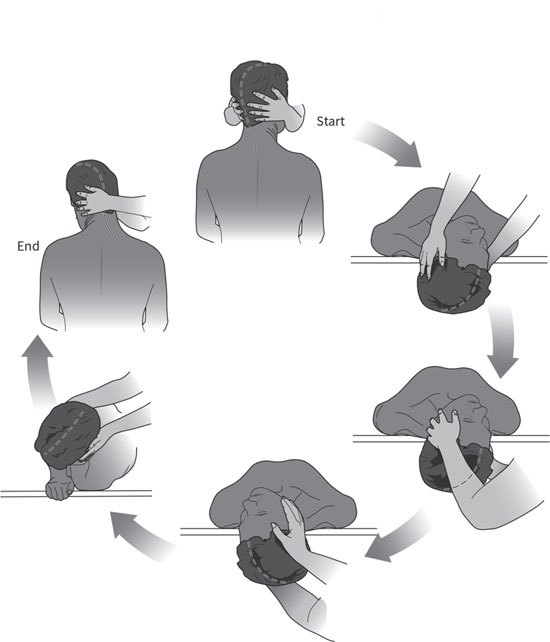

Further clinical reviews at one month, three months, six months and one year found that seven patients had suffered minor attacks of typical benign paroxysmal positional vertigo after three months. Three patients reported a major improvement in their vertigo, and their residual vertigo was relieved by performing the new manoeuvre again after two weeks. A new particle repositioning manoeuvre was designed for these patients, as an alternative to Epley's manoeuvre.Īt one week review, 36 patients (90 per cent) reported total relief from vertigo. This study included 40 patients complaining of vertigo and diagnosed as having benign paroxysmal positional vertigo. Such movements may not be wise in patients at risk of cervical spine fracture. Epley's manoeuvre necessitates passive neck movements. spondylosis and disc prolapse) are commoner in this age group. Benign paroxysmal positional vertigo can affect any age group but is commoner in older patients. The particle repositioning manoeuvre (Epley's manoeuvre) has become the 'gold standard' treatment for this disorder. Benign paroxysmal positional vertigo is one of the commonest peripheral vestibular causes of vertigo.
